Endometriosis: When Period Pain is More Than Just a Bad Period





Sunday, March 1st, 2026 - For millions of women globally, menstruation isn't simply an inconvenience; it's a debilitating experience that can severely impact their quality of life. While some discomfort is common, severe and persistent period pain should never be dismissed. Increasingly, medical professionals and patient advocates are sounding the alarm about endometriosis - a chronic, often underdiagnosed condition that can have profound consequences, particularly regarding fertility.
Beyond "Just a Bad Period": Understanding Endometriosis
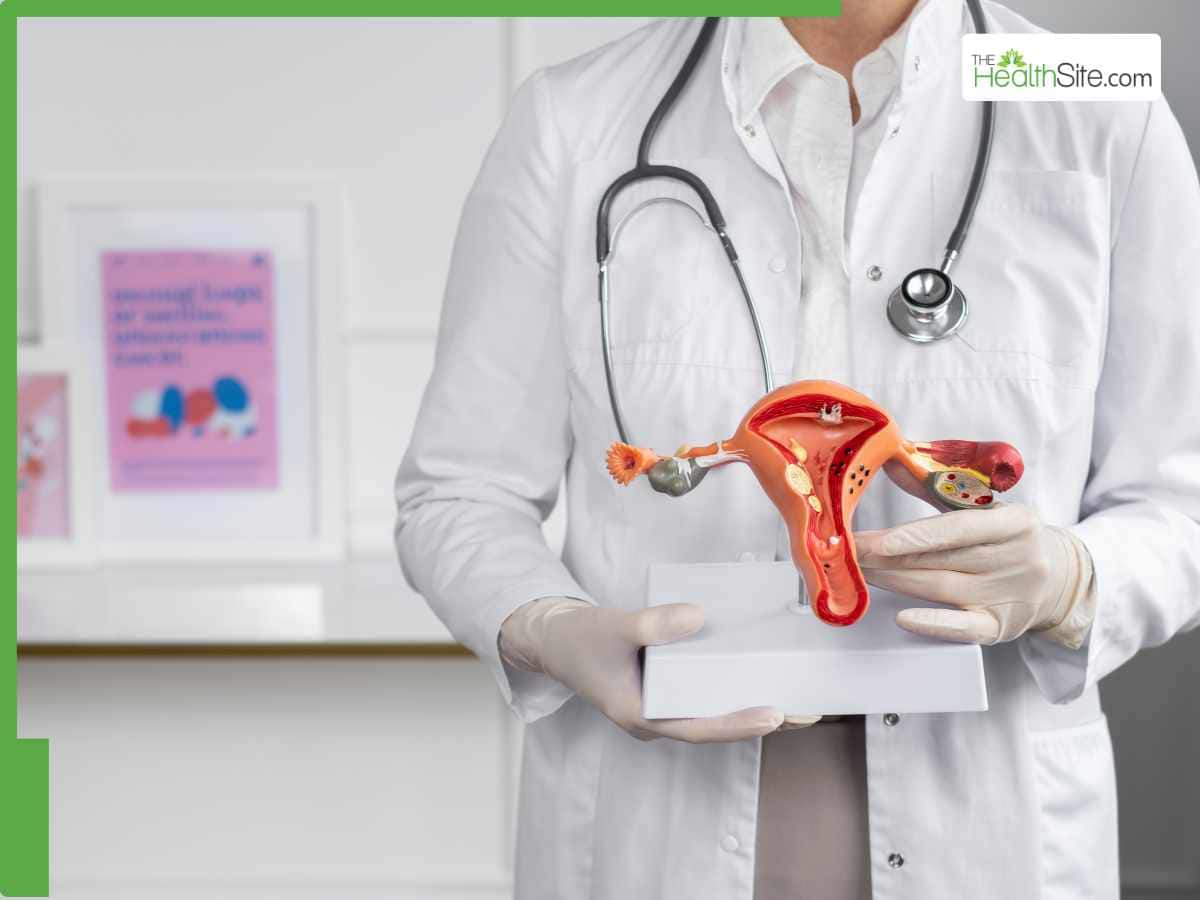
Endometriosis is characterized by the growth of tissue similar to the uterine lining (the endometrium) outside of the uterus. This misplaced tissue responds to hormonal fluctuations just like the uterine lining, thickening, breaking down, and bleeding with each menstrual cycle. The crucial difference? This blood and tissue have no natural exit route, leading to internal inflammation, scarring, and agonizing pain. The locations of these growths are diverse, found on the ovaries, fallopian tubes, bowel, bladder, and, in rare cases, even distant organs.
The Spectrum of Symptoms: Why Diagnosis is Often Delayed
The presentation of endometriosis varies dramatically from woman to woman. While some individuals experience mild discomfort, others are crippled by intense pain that disrupts their daily routines. Common symptoms include crippling menstrual cramps (dysmenorrhea), pain during or after sexual intercourse (dyspareunia), chronic pelvic pain that extends beyond menstruation, heavy or irregular bleeding, debilitating fatigue, and a range of digestive issues - bloating, diarrhea, constipation, and even nausea.
The wide range of symptoms, and their often non-specific nature, contributes significantly to the average diagnostic delay, which can be seven to ten years. This delay isn't merely frustrating; it's detrimental. Many women are told their pain is 'normal,' leading them to suffer in silence and delaying crucial medical intervention. A recent study published in the Journal of Women's Health highlighted that 60% of women surveyed reported feeling dismissed or minimized by healthcare professionals when describing their pain.
The Fertility Crisis: How Endometriosis Impacts Reproductive Health
The impact of endometriosis on fertility is a growing concern. The condition affects fertility through multiple mechanisms:
- Anatomical Distortion: Endometriotic growths can physically obstruct the fallopian tubes, preventing the sperm from reaching the egg and hindering fertilization.
- Inflammatory Environment: Chronic inflammation, a hallmark of endometriosis, creates a hostile environment within the pelvic cavity, damaging the ovaries, impacting egg quality, and disrupting the process of ovulation.
- Hormonal Disruption: Endometriosis can interfere with the delicate hormonal balance required for successful ovulation, implantation, and early pregnancy. Emerging research suggests endometriosis may even affect the receptivity of the uterine lining to implantation.
- Oxidative Stress: Studies are showing increased oxidative stress levels in the pelvic fluid of women with endometriosis, which can damage sperm and eggs.
Women with endometriosis often experience a longer time to conception and are significantly more likely to require assisted reproductive technologies (ART), such as in vitro fertilization (IVF), to achieve pregnancy. The financial, emotional, and physical toll of ART is substantial, and the success rates are often lower for women with endometriosis compared to those with other causes of infertility.
Diagnosis and Emerging Treatments
Diagnosing endometriosis remains a challenge. Currently, the gold standard for definitive diagnosis is laparoscopy - a minimally invasive surgical procedure allowing direct visualization of the pelvic organs. However, non-invasive diagnostic tools are being actively researched, including advanced imaging techniques and biomarker detection in blood or other bodily fluids. A recent clinical trial exploring a novel blood test showed promising results in identifying endometriosis with 85% accuracy, offering a potential avenue for earlier, less invasive diagnosis.
Treatment options are multifaceted and tailored to the individual's symptoms, disease severity, and reproductive goals. These include pain management strategies, hormonal therapies (birth control pills, GnRH agonists), laparoscopic surgical removal of endometriosis growths, and, in severe cases where childbearing is no longer desired, hysterectomy.
A Call to Action: Breaking the Silence and Improving Care
It's time to dismantle the stigma surrounding menstrual pain and empower women to advocate for their health. Increased awareness among healthcare professionals, improved diagnostic tools, and a shift in societal perceptions are crucial. Don't dismiss severe period pain. Demand answers. Early diagnosis and proactive management can significantly improve your quality of life and preserve your reproductive potential. Resources like the Endometriosis Foundation of America (https://www.endofound.org/) and the World Endometriosis Research Foundation (https://www.werf.org/) offer valuable information and support.
Read the Full TheHealthSite Article at:
https://www.thehealthsite.com/pregnancy/endometriosis-explained-why-severe-period-pain-should-never-be-ignored-and-how-delayed-diagnosis-impacts-fertility-1301168/
on: Tue, Feb 24th
by: TheHealthSite

on: Mon, Feb 23rd
by: TheHealthSite

on: Sat, Feb 21st
by: TheHealthSite

on: Thu, Feb 19th
by: TheHealthSite

on: Mon, Feb 16th
by: TheHealthSite

on: Sun, Feb 15th
by: TheHealthSite

on: Sat, Jan 31st
by: TheHealthSite

on: Thu, Jan 15th
by: TheHealthSite

on: Sun, Jan 11th
by: Onlymyhealth
Skinny Jeans & Shapewear Linked to Reproductive Health Risks

on: Fri, Dec 19th 2025
by: TheHealthSite
Fertility Health Resolutions 2026: A Couples' Guide to Pre-Conception Wellness

on: Fri, Dec 12th 2025
by: TheHealthSite
PCOD vs PCOS: Understanding the Real Differences and Their Impact on Pregnancy

on: Thu, May 01st 2025
by: TheHealthSite
Case Study: How A 29-Year-Old Woman Overcame Severe Endometriosis Pain And 'Kissing Ovaries'