Massachusetts Implements Medicaid Work Requirement





Boston, MA - March 2nd, 2026 - Massachusetts's ambitious and hotly debated Medicaid work requirement policy officially rolled out statewide this week, marking a significant shift in the state's approach to public health coverage. The policy, requiring most able-bodied adults aged 19-64 to prove 20 hours of weekly engagement in work, volunteering, job training, or education to maintain Medicaid eligibility, is already facing scrutiny and promises to reshape access to healthcare for thousands of residents.
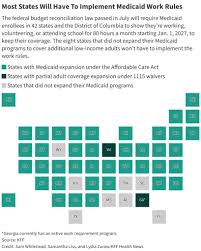
This move places Massachusetts among a growing number of states experimenting with similar provisions, often framed as a means of promoting self-sufficiency and controlling escalating Medicaid costs. However, critics argue these requirements create unnecessary barriers to care, disproportionately impacting vulnerable populations and potentially worsening health outcomes. The implementation follows a phased approach, starting with pilot programs in several counties over the past year, allowing the state to gather data and refine its outreach efforts.
The Rationale Behind the Policy:
Governor Healey and her administration maintain the policy is fiscally responsible. Massachusetts, like many states, faces substantial pressure on its Medicaid budget, officially known as MassHealth. The state projects the work requirement will generate significant savings, though precise figures remain contested. Proponents argue that by encouraging participation in the workforce or community service, the policy not only reduces the financial burden on taxpayers but also fosters greater individual independence and economic stability among Medicaid recipients. The underlying philosophy is that maintaining coverage should be tied, where possible, to active engagement in activities that contribute to personal and societal well-being.
Who is Affected and Who is Exempt?
The policy's scope is broad, encompassing a large segment of the Medicaid population. However, several exemptions exist. Individuals with disabilities, pregnant women, and those caring for dependent children are shielded from the requirement. Additionally, exemptions are available for those participating in substance abuse treatment programs or facing significant barriers to employment, such as lack of transportation or childcare. The state has created a complex verification system, utilizing online portals and case managers to assess eligibility and track reported hours.
Legal Battles and Advocacy Concerns:
The implementation hasn't been without opposition. Multiple lawsuits have been filed by advocacy groups arguing the policy violates federal Medicaid regulations and constitutes an unreasonable barrier to access to care. These groups contend that the requirement creates administrative hurdles that disproportionately affect individuals with limited resources, those with mental health conditions, and people living in rural areas with limited job opportunities. They also highlight the potential for increased uninsurance rates and delayed medical care, leading to more expensive health crises down the line.
"We're deeply concerned about the impact this will have on our clients," says Sarah Chen, Executive Director of the Massachusetts Coalition for the Homeless. "Many of the individuals we serve face significant challenges finding and maintaining employment, and this policy adds another layer of complexity to an already difficult situation. We predict a significant number of people will lose coverage, not because they don't need healthcare, but because they can't navigate the bureaucratic requirements."
The Outreach Effort and Support Services:
Recognizing the potential challenges, the state has invested in a robust outreach program to inform Medicaid recipients about the new rules. This includes mailings, public service announcements, and community workshops. The state has also partnered with local organizations to provide support services, such as job search assistance, resume writing workshops, and volunteer placement. The success of these efforts will be crucial in mitigating the negative consequences of the policy and ensuring that those who are genuinely unable to meet the requirements receive the necessary support. There is a dedicated hotline and online resource center to address questions and concerns.
Looking Ahead: Long-Term Impacts and National Implications:
The long-term effects of Massachusetts's Medicaid work requirement remain to be seen. The state will be closely monitoring enrollment numbers, healthcare utilization rates, and the impact on vulnerable populations. The results of this experiment could have significant implications for other states considering similar policies. The Biden administration has signaled a willingness to allow states to pursue innovative approaches to Medicaid, but with a focus on ensuring access to care. The Massachusetts case will serve as a key test of the balance between fiscal responsibility and the fundamental right to healthcare. Analysts are watching closely to see if the projected savings materialize, and whether the policy truly promotes self-sufficiency, or simply shifts healthcare costs onto other parts of the system.
Read the Full Boston Herald Article at:
https://www.bostonherald.com/2026/02/24/new-medicaid-work-rules/
on: Wed, Feb 25th
by: Orlando Sentinel
Florida's Medicaid Work Requirements Face Unintended Consequences

on: Wed, Feb 25th
by: Daily Camera
on: Tue, Feb 24th
by: Los Angeles Daily News
California Debates Governor Reynolds' Medi-Cal Work Requirements

on: Tue, Feb 24th
by: Sun Sentinel

on: Tue, Feb 24th
by: The Baltimore Sun

on: Mon, Feb 16th
by: MassLive

on: Sat, Feb 28th
by: The Nation

on: Sat, Feb 28th
by: TwinCities.com

on: Tue, Feb 24th
by: East Bay Times
California's Medicaid Work Requirements Face Legal Challenge

on: Sat, Feb 28th
by: Patch

on: Tue, Feb 24th
by: Hartford Courant

on: Tue, Feb 17th
by: New Jersey Monitor
Millions at Risk: Medicaid Unwinding Threatens Healthcare Access