Connecticut Medicaid Work Requirements Paused by Court





Hartford, CT - February 25, 2026 - Connecticut's ambitious, yet controversial, attempt to tie Medicaid eligibility to work requirements has hit a major snag. A Hartford Superior Court judge issued a preliminary injunction yesterday, February 24th, effectively pausing the implementation of rules that demanded recipients document 20 hours of weekly activity - encompassing employment, volunteering, or job training - to maintain their healthcare coverage. This legal challenge, brought forth by a coalition of advocacy groups, throws the future of the policy into uncertainty and sparks a crucial debate about the balance between promoting self-sufficiency and ensuring access to vital healthcare for vulnerable populations.
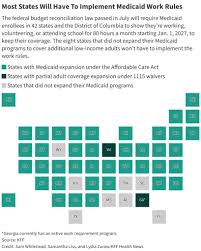
The policy, which was briefly active from February 15th, 2026, represents a nationwide trend gaining momentum in several states. Proponents argue that attaching work requirements to public assistance programs incentivizes individuals to seek employment, ultimately reducing dependence on government aid and bolstering the economy. Governor Evelyn Reed, a staunch supporter of the initiative, framed the requirements as a necessary measure for "fiscal responsibility and promoting a pathway to self-sufficiency" in a statement released late Tuesday. She expressed her disappointment with the injunction and reaffirmed her commitment to defending the policy in court.
However, the implementation, even in its short-lived initial phase, was plagued with issues. Advocacy groups immediately voiced concerns regarding accessibility and the potential for disenfranchisement. Sarah Miller, lead counsel for the plaintiffs, described the rollout as "chaotic" and the state's outreach efforts as "demonstrably insufficient." The primary complaint centers around a lack of adequate preparation and support for recipients navigating the new system, specifically the online portal created by the Department of Social Services (DSS) to verify compliance. Many recipients, Miller argues, were simply unaware of the new rules, lacked the technological resources to access the portal, or encountered significant difficulties understanding and fulfilling the requirements.
The lawsuit isn't simply a critique of implementation; it challenges the fundamental legality and ethical implications of the policy itself. Central to the plaintiffs' argument is the claim that the work requirements disproportionately impact marginalized communities. This includes individuals with disabilities who may face significant barriers to employment, caregivers responsible for children or elderly relatives, and those living in areas with limited job opportunities. Critics argue that denying healthcare to these individuals based on their inability to meet the work requirements is not only unjust but also counterproductive, potentially leading to poorer health outcomes and increased healthcare costs in the long run.
This case echoes similar legal battles unfolding across the country. Arkansas, for instance, experienced a significant reduction in Medicaid enrollment after implementing similar work requirements, a move that was subsequently overturned by a federal judge. Kentucky's attempt to implement work requirements also faced legal challenges and was ultimately blocked. These precedents weigh heavily on the Connecticut case, highlighting the legal and logistical hurdles associated with such policies. The core question consistently revolves around the extent to which states can impose conditions on federal benefits, and whether those conditions align with the underlying purpose of the programs - in this case, ensuring access to healthcare.
Beyond the legal arguments, the policy raises broader questions about the nature of work and its relationship to healthcare. Should access to essential healthcare be contingent upon participation in the formal labor market? Does focusing solely on "work" undervalue other forms of meaningful contribution to society, such as volunteering or caregiving? These are complex questions with no easy answers, and the Connecticut case is likely to fuel a national conversation about the social safety net and the role of government in providing healthcare to its citizens.
The upcoming hearing, scheduled for April 2026, will be crucial in determining the fate of Connecticut's Medicaid work requirements. The judge will need to weigh the state's arguments for self-sufficiency against the plaintiffs' concerns about equity and access to healthcare. The outcome of this case will not only impact the thousands of Connecticut residents currently enrolled in Medicaid but also set a precedent for other states considering similar policies. It's a battle that speaks to the heart of America's ongoing struggle to balance individual responsibility with the collective obligation to care for its most vulnerable citizens.
Read the Full Hartford Courant Article at:
https://www.courant.com/2026/02/24/new-medicaid-work-rules/
on: Mon, Feb 23rd
by: Patch

on: Mon, Feb 23rd
by: Orange County Register

on: Sat, Feb 21st
by: inforum
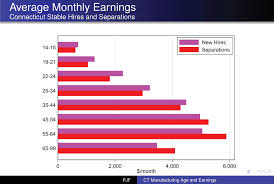
Connecticut Manufacturing Faces Critical Skilled Labor Shortage
on: Fri, Feb 20th
by: Utah News Dispatch
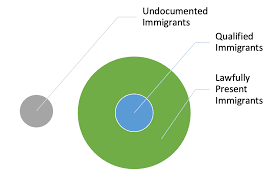
Arizona Bill Restricts Healthcare for Undocumented Children, Sparks Outrage
on: Fri, Feb 20th
by: TwinCities.com

on: Tue, Feb 17th
by: New Jersey Monitor
Millions at Risk: Medicaid Unwinding Threatens Healthcare Access

on: Sat, Feb 14th
by: Hartford Courant
Kennedy Health System Faces Transparency Scrutiny After Damning Report

on: Wed, Feb 11th
by: Kentucky Lantern
Kentucky's Public Notice Lawsuit: Tradition vs. Digital Access

on: Tue, Feb 10th
by: The Independent US

on: Sat, Feb 07th
by: Idaho Capital Sun

on: Sat, Jan 31st
by: stacker