[ Wed, Feb 25th ]: Times of San Diego
[ Wed, Feb 25th ]: Heavy.com
[ Wed, Feb 25th ]: Polygon
[ Wed, Feb 25th ]: The Columbian
[ Wed, Feb 25th ]: U.S. News & World Report
[ Wed, Feb 25th ]: Post and Courier
[ Wed, Feb 25th ]: WTOP News
[ Wed, Feb 25th ]: KEZI
[ Wed, Feb 25th ]: Atlanta Blackstar
[ Wed, Feb 25th ]: The Oakland Press
[ Wed, Feb 25th ]: South Florida Sun Sentinel
[ Wed, Feb 25th ]: Seattle Times
[ Wed, Feb 25th ]: Daily Mail
[ Wed, Feb 25th ]: syracuse.com
[ Wed, Feb 25th ]: WHNT Huntsville
[ Wed, Feb 25th ]: The Center Square
[ Wed, Feb 25th ]: Sporting News
[ Wed, Feb 25th ]: RTE Online
[ Wed, Feb 25th ]: The New Indian Express
[ Wed, Feb 25th ]: dw
[ Wed, Feb 25th ]: Yen.com.gh
[ Wed, Feb 25th ]: Birmingham Mail
[ Wed, Feb 25th ]: NewsNation
[ Wed, Feb 25th ]: Reuters
[ Wed, Feb 25th ]: Pharmaceutical Technology
[ Wed, Feb 25th ]: The Messenger
[ Wed, Feb 25th ]: yahoo.com
[ Wed, Feb 25th ]: New Jersey Monitor
[ Wed, Feb 25th ]: ABC15 Arizona
[ Wed, Feb 25th ]: IBTimes UK
[ Wed, Feb 25th ]: Palm Beach Post
[ Wed, Feb 25th ]: CNN
[ Wed, Feb 25th ]: The Hill
[ Wed, Feb 25th ]: NBC 10 Philadelphia
[ Wed, Feb 25th ]: Daily Camera
[ Wed, Feb 25th ]: Patch
[ Wed, Feb 25th ]: ABC News
[ Wed, Feb 25th ]: TheHealthSite
[ Wed, Feb 25th ]: WJTV Jackson
[ Tue, Feb 24th ]: Hartford Courant
[ Tue, Feb 24th ]: Toronto Star
[ Tue, Feb 24th ]: Sporting News
[ Tue, Feb 24th ]: Newsweek
[ Tue, Feb 24th ]: BBC
[ Tue, Feb 24th ]: Penn Live
[ Tue, Feb 24th ]: Fox News
[ Tue, Feb 24th ]: The Conversation
[ Tue, Feb 24th ]: TheHealthSite
Colorado's Medicaid Work Requirements Face Legal Challenge
Locale: UNITED STATES
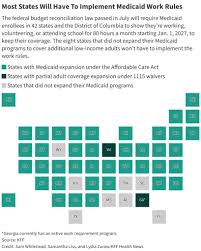




Denver, CO - February 25, 2026 - Colorado's ambitious and controversial implementation of Medicaid work requirements is facing escalating legal challenges and sparking a heated public debate, raising critical questions about access to healthcare for vulnerable populations. Just weeks after the rules officially took effect, a major lawsuit threatens to halt the program, while advocates and state officials clash over its efficacy and fairness.
The policy, a key initiative of Governor Amelia Stone's administration, requires most adult Medicaid recipients without dependent children to prove they are actively engaged in work, volunteer service, or approved job training programs to retain their healthcare coverage. Proponents argue this fosters self-sufficiency and responsible use of taxpayer dollars, aligning with a national trend towards increased accountability within social safety nets. However, opponents contend the requirements are punitive, discriminatory, and ultimately harmful to those who rely on Medicaid for essential healthcare services.
Last week's lawsuit, spearheaded by Colorado Legal Services alongside disability rights groups like Access Colorado and the Rural Healthcare Coalition, alleges the rules violate both the spirit and letter of federal Medicaid law. The plaintiffs argue the requirements create unnecessary and often insurmountable hurdles for individuals already facing significant challenges, including disabilities (both physical and mental), lack of reliable transportation, limited access to childcare, and geographical barriers in rural communities.
"The state is effectively punishing people for being poor and vulnerable," explains Sarah Chen, lead attorney for Colorado Legal Services. "These rules aren't designed to help people find work; they're designed to reduce enrollment in Medicaid, period. The administrative burden alone is crippling. We're seeing clients who are genuinely trying to comply but are getting lost in a complex bureaucratic system." Chen's organization points to examples of individuals with chronic health conditions struggling to meet hourly requirements, and rural residents lacking access to consistent internet service needed to report their activities through the state's online portal.
The Department of Health Care Policy and Finance (DHCPF) maintains the policy is a necessary step towards promoting workforce participation and long-term financial stability. DHCPF Director, Dr. Emily Carter, defended the regulations in a press conference yesterday, stating, "We've invested significantly in resources to support beneficiaries in meeting these requirements, including job search assistance, transportation vouchers, and accessible training programs. We believe this policy empowers individuals to take control of their lives and achieve greater independence." However, critics highlight that these resources are severely underfunded and overwhelmed by demand, particularly in less populated areas.
Initial data released by the DHCPF estimates approximately 300,000 Colorado adults could be affected by the new rules. The state projects a modest decrease in Medicaid enrollment - roughly 5-7% - but acknowledges that these figures are preliminary and subject to change pending the outcome of the legal challenges. Experts warn that even a small reduction in enrollment could have significant consequences for Colorado's healthcare system, potentially increasing strain on emergency rooms and other safety-net providers.
The debate in Colorado mirrors a national conversation about the future of Medicaid and the role of work requirements in social welfare programs. Similar policies have been implemented in other states, with mixed results. Some studies suggest that work requirements have minimal impact on employment rates but lead to significant disenrollment from Medicaid, particularly among vulnerable populations. Other studies point to potential benefits, such as increased earnings for those who do find work.
The Colorado case is being closely watched by advocacy groups and policymakers across the country. The court is expected to hear arguments in early April, and legal analysts predict a lengthy and complex process. The ruling will not only determine the fate of Colorado's Medicaid work requirements but could also set a precedent for similar policies in other states. Beyond the legal ramifications, the ongoing debate underscores the fundamental tension between fiscal responsibility and ensuring access to healthcare for all, particularly those most in need. The long-term consequences for Colorado's most vulnerable populations - and the future of Medicaid itself - remain uncertain.
Read the Full Daily Camera Article at:
https://www.dailycamera.com/2026/02/24/new-medicaid-work-rules/
[ Tue, Feb 24th ]: Hartford Courant
[ Tue, Feb 24th ]: Los Angeles Daily News
[ Tue, Feb 24th ]: Sun Sentinel
[ Tue, Feb 24th ]: The Baltimore Sun
[ Tue, Feb 24th ]: East Bay Times
[ Tue, Feb 24th ]: Daily Press
[ Mon, Feb 23rd ]: Orange County Register
[ Fri, Feb 20th ]: TwinCities.com
[ Sun, Feb 15th ]: Sun Sentinel
[ Tue, Feb 10th ]: The Denver Post
[ Thu, Feb 05th ]: Bangor Daily News
[ Sat, Jan 31st ]: stacker