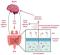
Rising Tide: Pediatric Hypertension on the Rise in the United States
 TheHealthSite
TheHealthSiteLocale:





Hypertension in Kids: Why Early Detection Matters and How to Stop a Silent Health Crisis
For decades, high blood pressure (hypertension) has been the quintessential adult‑centric disease. It was almost unheard of in children—until recent decades, when data began to show a silent rise in the condition among the young. The article on TheHealthSite.com titled “Hypertension in Kids: Know the Leading Cause of This Silent Health Crisis & Prevent Mid‑Life Heart Disease” dives into the epidemiology, risk factors, and most importantly, the practical steps parents, pediatricians, and schools can take to reverse the trend. Below is a detailed summary of that piece, including additional context from linked resources that enrich our understanding of pediatric hypertension.
1. The Rising Tide: Epidemiology of Pediatric Hypertension
- Prevalence: According to the article, roughly 1–2 % of children in the United States have diagnosed hypertension, but recent estimates suggest that the real number could be higher, especially among those who are overweight or belong to certain ethnic groups.
- Silent Progression: Most children with high blood pressure are asymptomatic, earning the label “silent crisis.” Without routine screening, the condition can progress unnoticed until adulthood.
- Long‑Term Consequences: Elevated blood pressure in childhood tracks into adulthood, raising the risk of heart disease, stroke, kidney disease, and even cognitive decline later in life. A key point the article emphasizes is that the “childhood origins” of cardiovascular disease are a major driver of the national burden of chronic illness.
2. The Leading Cause: Obesity and the Diet‑Exercise Connection
The piece identifies childhood obesity as the leading modifiable cause of hypertension in kids, linking it to excess salt intake and reduced physical activity.
- Salt & Sodium: An online link in the article directs readers to the American Heart Association page on sodium intake (https://www.heart.org). There, experts recommend less than 1,500 mg of sodium per day for children aged 2–8, and 1,500–2,300 mg for those 9–18.
- Obesity: The article cites a study in Pediatrics that shows children who are obese are 3–4 times more likely to have hypertension compared to their normal‑weight peers.
- Physical Activity: The American Academy of Pediatrics (AAP) recommends at least 60 minutes of moderate‑to‑vigorous activity daily. The TheHealthSite article notes that kids who meet this guideline have a 30 % lower risk of developing hypertension.
3. Screening: When and How to Measure Blood Pressure
The article details the current AAP screening guidelines, which were updated in 2017:
- Age‑Based Initiation: Screening should begin at age 3, with a confirmatory test in two separate visits.
- Blood Pressure Categories: Children’s blood pressure is compared against percentiles for age, sex, and height.
- Clinic Measurements: The article links to CDC’s blood pressure measurement guidelines (https://www.cdc.gov/bloodpressure) that stress proper cuff sizing, correct positioning, and multiple readings to reduce error.
4. The Silent “Hypertension Crisis”—A Multi‑Layered Response
The article frames pediatric hypertension not just as a medical issue but as a social one. It calls for a coordinated approach involving:
- Schools: Implementing nutrition and exercise curricula that reduce sodium exposure and promote daily activity.
- Primary Care: Routine blood pressure checks, family education, and early intervention with lifestyle counseling.
- Policy: Advocacy for lower sodium in processed foods and improved access to fresh produce.
5. Treatment Options: Lifestyle First, Medications Second
When lifestyle changes are insufficient, the article outlines pharmacologic options, drawing on the American College of Cardiology/Heart Association (ACC/AHA) guidelines (https://www.acc.org). Key takeaways:
- First‑Line Drugs: ACE inhibitors, ARBs, calcium channel blockers, or thiazide diuretics, depending on patient age and comorbidities.
- Monitoring: Regular follow‑ups to track blood pressure and potential side‑effects.
- Duration: In many cases, once healthy weight and diet are achieved, medication can be tapered or discontinued, but long‑term monitoring remains essential.
6. Prevention: A Multi‑Faceted Strategy
The article underscores prevention as the cornerstone. The integrated plan includes:
Nutrition
- Reduce sodium: Avoid processed snacks, canned soups, and fast‑food.
- Increase potassium: Fruits and vegetables help counteract sodium effects.
- Promote whole grains and lean proteins.Physical Activity
- Structured play: Sports, dance, and active games.
- Reduce sedentary screen time to less than 2 hours per day.Weight Management
- Use growth charts and BMI percentiles to monitor progress.
- Family‑based interventions increase success rates.Stress Management
- Mind‑body techniques, adequate sleep (9–12 hours per night for children), and healthy coping strategies.Regular Health Checks
- Annual pediatric visits should include blood pressure screening for kids over 3 years old.
7. The Role of Family History and Genetics
The article cites research indicating a strong familial component to pediatric hypertension. A parent with high blood pressure increases a child’s risk by about 50 %. Genetic predisposition can also influence salt sensitivity and the renin‑angiotensin‑aldosterone system. In such cases, early lifestyle interventions are especially critical.
8. Future Directions: Research and Public Health Initiatives
- Technology: Wearable blood pressure monitors and tele‑health platforms are being trialed to enhance monitoring.
- Policy: The article highlights ongoing legislative efforts to limit sodium in school meals and to fund community sports programs.
- Education: The AAP recommends educational campaigns targeting both parents and children, fostering a culture of health.
9. Bottom Line: Early Action Saves Lives
The piece’s central thesis is that pediatric hypertension is a silent health crisis that can be curbed with early detection and lifestyle changes. The longer hypertension remains untreated in a child, the greater the cumulative damage to the cardiovascular system. By implementing the AAP’s screening guidelines, promoting a diet low in sodium, encouraging regular exercise, and addressing obesity, we can intercept hypertension early and dramatically reduce the risk of mid‑life heart disease.
Quick Reference
| Step | Action | Reference |
|---|---|---|
| Screen | Blood pressure measurement at age 3 and confirmatory readings | AAP guidelines |
| Measure | Use proper cuff size; at least 3 readings | CDC guidelines |
| Reduce Salt | <1,500 mg/day for 2–8 yrs; <2,300 mg/day for 9–18 yrs | AHA |
| Increase Activity | ≥60 min/day of moderate/vigorous activity | AAP |
| Monitor Weight | BMI percentile tracking | Pediatric growth charts |
| Treat | Lifestyle first; medication if needed | ACC/AHA |
Final Thought
The health of tomorrow’s adults begins in the classrooms, playgrounds, and bedrooms of today. By recognizing that hypertension in kids is not a trivial footnote but a major public‑health issue, we empower ourselves to take the steps that will keep our children—and our communities—healthy for decades to come.
Read the Full TheHealthSite Article at:
[ https://www.thehealthsite.com/diseases-conditions/hypertension-in-kids-know-the-leading-cause-of-this-silent-health-crisis-prevent-midlife-heart-disease-1267658/ ]