[ Wed, Feb 25th ]: The Hill
[ Wed, Feb 25th ]: NBC 10 Philadelphia
[ Wed, Feb 25th ]: Daily Camera
[ Wed, Feb 25th ]: Patch
[ Wed, Feb 25th ]: ABC News
[ Wed, Feb 25th ]: TheHealthSite
[ Wed, Feb 25th ]: WJTV Jackson
[ Tue, Feb 24th ]: CNET
[ Tue, Feb 24th ]: Hartford Courant
[ Tue, Feb 24th ]: nbcnews.com
[ Tue, Feb 24th ]: Los Angeles Daily News
[ Tue, Feb 24th ]: Toronto Star
[ Tue, Feb 24th ]: WKRG
[ Tue, Feb 24th ]: Washington Examiner
[ Tue, Feb 24th ]: Sporting News
[ Tue, Feb 24th ]: Austin American-Statesman
[ Tue, Feb 24th ]: WHIO
[ Tue, Feb 24th ]: WLNS Lansing
[ Tue, Feb 24th ]: Newsweek
[ Tue, Feb 24th ]: Penn Live
[ Tue, Feb 24th ]: TheNewsCenter
[ Tue, Feb 24th ]: Sun Sentinel
[ Tue, Feb 24th ]: reuters.com
[ Tue, Feb 24th ]: Dallas Morning News
[ Tue, Feb 24th ]: The Baltimore Sun
[ Tue, Feb 24th ]: East Bay Times
[ Tue, Feb 24th ]: The Denver Post
[ Tue, Feb 24th ]: WRDW
[ Tue, Feb 24th ]: Her Campus
[ Tue, Feb 24th ]: The Conversation
[ Tue, Feb 24th ]: yahoo.com
[ Tue, Feb 24th ]: Daily Press
[ Tue, Feb 24th ]: Heavy.com
[ Tue, Feb 24th ]: Patch
[ Tue, Feb 24th ]: Daily
[ Tue, Feb 24th ]: rnz
[ Tue, Feb 24th ]: Fox News
[ Tue, Feb 24th ]: Global News
[ Tue, Feb 24th ]: The Cool Down
[ Tue, Feb 24th ]: New Jersey Monitor
[ Tue, Feb 24th ]: WTOP News
[ Tue, Feb 24th ]: Seattle Times
[ Tue, Feb 24th ]: The Mirror
[ Tue, Feb 24th ]: The Independent
[ Tue, Feb 24th ]: Staten Island Advance
[ Tue, Feb 24th ]: TheHealthSite
[ Tue, Feb 24th ]: NBC News
[ Tue, Feb 24th ]: BBC
Women's Health Tech Fails: A Critical Gap
 yahoo.com
yahoo.comLocale: UNITED STATES
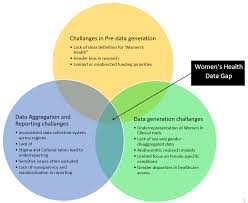




Beyond the Cycle: The Urgent Need for Truly Personalized Women's Health Tech
Wearable technology has become ubiquitous, adorning wrists and offering a constant stream of data about our daily activity, sleep patterns, and heart rates. While marketed as tools for empowerment and proactive health management, a critical gap persists: these devices consistently underperform when applied to women's health. Today, February 24th, 2026, the conversation is shifting from simply acknowledging this shortcoming to demanding a fundamental rethink of how women's health technology is designed, developed, and integrated into healthcare systems.
The core issue isn't the technology itself, but the assumption of universality. For decades, medical research - and consequently, the algorithms powering many wearables - has been heavily biased towards male physiology. The female body, however, is a dynamic landscape sculpted by complex hormonal cycles, reproductive stages, and individual biological variations. "The range of normal for women is much wider than it is for men," explains Dr. Maria Shriver of UCLA Health, a sentiment echoed by a growing number of female-focused healthcare advocates. "What's normal for one woman might be completely abnormal for another."
This inherent variability presents a significant challenge for standardized wearable metrics. A resting heart rate that triggers an alert on a male-centric algorithm might be perfectly normal for a woman during a specific phase of her menstrual cycle, or during perimenopause. Similarly, sleep tracking can be skewed by hormonal fluctuations that impact sleep architecture, leading to inaccurate assessments of restfulness and potential misdiagnosis of sleep disorders. Existing menstrual cycle tracking features, often reliant on manual input, offer a limited, and often incomplete, picture. They fail to capture the nuanced impact of hormones on a wider range of physiological processes.
The problem extends beyond reproductive health. Conditions like autoimmune diseases - disproportionately affecting women - often present with subtle, fluctuating symptoms that current wearables are ill-equipped to detect. The lack of granular data and personalized baselines means that early warning signs can be missed, delaying diagnosis and potentially impacting treatment outcomes. Furthermore, the "one-size-fits-all" approach overlooks the interplay between lifestyle factors, genetics, and hormonal influences - creating a system that often generates more noise than signal.
Fortunately, a new wave of companies is recognizing this critical need and developing more specialized wearables designed specifically for women. These devices aim to move beyond basic cycle tracking and incorporate sensors capable of monitoring hormonal levels through non-invasive methods (like sweat or interstitial fluid analysis), tracking key reproductive health markers, and analyzing data with algorithms trained on diverse female datasets. Some are even exploring the integration of biomarkers to detect early signs of conditions like endometriosis or polycystic ovary syndrome (PCOS).
However, significant hurdles remain. Data privacy and security are paramount, especially when dealing with sensitive reproductive and hormonal information. Ensuring the robust encryption and responsible handling of this data is crucial to building trust and encouraging widespread adoption. Affordability and accessibility are also key considerations. These specialized devices must be priced competitively and available to women of all socioeconomic backgrounds to truly bridge the healthcare gap.
Perhaps most importantly, technology cannot operate in a vacuum. Dr. Shriver emphasizes the need for a holistic approach, integrating wearable data with the expertise of medical professionals. "Wearables can be a useful tool, but they're not a substitute for seeing a doctor," she states. "We need to integrate these devices into a broader healthcare system that provides women with the support and guidance they need to make informed decisions about their health." This means developing user-friendly interfaces for healthcare providers to interpret wearable data effectively, as well as establishing clear guidelines for data interpretation and clinical application.
Looking ahead, the future of women's health tech lies in personalized algorithms, continuous monitoring, and a collaborative approach between technology developers, healthcare providers, and, most importantly, the women themselves. The conversation is evolving beyond simply tracking cycles to understanding the intricate biological rhythms that define the female experience. This isn't just about creating better gadgets; it's about finally addressing a long-standing inequity in healthcare and empowering women with the tools they need to truly understand and manage their well-being.
Read the Full yahoo.com Article at:
https://tech.yahoo.com/wearables/articles/women-health-too-complex-one-140000417.html
[ Fri, Feb 20th ]: Time
[ Tue, Feb 17th ]: yahoo.com
[ Mon, Feb 16th ]: The Hans India
[ Mon, Feb 16th ]: The Irish News
[ Tue, Feb 10th ]: yahoo.com
[ Mon, Feb 09th ]: WVUE FOX 8 News
[ Sat, Feb 07th ]: Impacts
[ Sat, Feb 07th ]: yahoo.com
[ Fri, Feb 06th ]: yahoo.com
[ Thu, Feb 05th ]: TheHealthSite
[ Thu, Feb 05th ]: yahoo.com
[ Thu, Jan 15th ]: FOX13 Memphis