Yale New Haven Health, Anthem Reach Agreement, Restoring Healthcare Access





NEW HAVEN, Conn. (February 26th, 2026) - Yale New Haven Health (YNHH) and Anthem Blue Cross and Blue Shield have officially ratified a new agreement, resolving a contentious standoff that threatened access to critical healthcare services for Anthem members across Connecticut. The deal, finalized earlier today, restores full network access for Anthem policyholders to all YNHH hospitals and associated facilities, bringing an end to weeks of uncertainty and disruption.
The dispute, which initially surfaced in December 2025, highlighted the increasingly strained relationship between major hospital systems and insurance providers. At its core, the conflict revolved around reimbursement rates and contract stipulations - a now-familiar battleground in the evolving landscape of American healthcare financing. The temporary lapse in coverage forced patients to delay non-emergency appointments and procedures, creating both individual anxieties and systemic bottlenecks within the healthcare system.
This isn't an isolated incident. Over the past five years, similar disputes have erupted between insurers and providers nationwide, often reaching similarly precarious tipping points. The YNHH-Anthem clash gained particular attention due to the prominence of both organizations and the potential impact on a large swathe of the Connecticut population. Experts suggest this resolution, while welcomed, likely represents a compromise rather than a complete victory for either side.
Beyond Reimbursement: The Larger Healthcare Sustainability Issue
The immediate cause of the disagreement - acceptable reimbursement rates - masked deeper concerns about the long-term sustainability of healthcare provision. YNHH maintained that Anthem's proposed rates failed to adequately cover the rising costs of delivering high-quality care, citing factors such as increasing labor expenses, the price of advanced medical technologies, and the growing demand for specialized services. Anthem, on the other hand, argued that YNHH was requesting unsustainable rate hikes that would ultimately be passed onto consumers in the form of higher premiums.
These arguments reflect a broader trend: hospitals, particularly those with significant investments in specialized care and teaching programs like YNHH, face mounting financial pressures. They contend that traditional fee-for-service models incentivize volume over value and fail to recognize the true cost of complex medical interventions. Insurance companies, meanwhile, are under pressure to control costs and demonstrate value to their shareholders and policyholders. The delicate balance between these competing priorities is becoming increasingly difficult to maintain.
The Terms Remain Secret, But the Implications are Clear
While the specifics of the agreement remain confidential, both YNHH spokesperson Mark Taylor and Anthem officials released statements acknowledging a "mutually beneficial" outcome. Taylor stated, "We are pleased to announce that we have reached a mutually beneficial agreement with Anthem Blue Cross and Blue Shield." Anthem's statement echoed this sentiment, declaring, "This agreement is a testament to our commitment to ensuring access to high-quality, affordable care for our members while supporting the financial viability of our provider partners."
The lack of transparency surrounding the financial details is not unusual in these types of negotiations. However, analysts believe the agreement likely includes a multi-year rate structure with built-in adjustments for inflation and changes in the cost of care. It's also probable that the deal incorporates provisions for value-based care initiatives, where reimbursement is tied to patient outcomes rather than simply the volume of services provided.
A Potential Model for Future Negotiations?
Experts are closely watching this resolution to see if it can serve as a template for future negotiations between hospital systems and insurance providers. The key takeaway might be the necessity for proactive, long-term agreements that address the underlying structural issues driving up healthcare costs. Simply patching up short-term disagreements is no longer a viable solution.
Furthermore, the rise of consumer-directed healthcare and the increasing demand for price transparency are forcing both insurers and providers to rethink their negotiating strategies. Patients are becoming more engaged in their healthcare decisions and are demanding greater clarity about the costs of their care. This trend is likely to intensify in the coming years, further complicating the already complex dynamics of healthcare financing.
Ultimately, the YNHH-Anthem agreement offers a temporary reprieve for patients and providers alike. However, the fundamental challenges facing the American healthcare system remain. Addressing these challenges will require a concerted effort from all stakeholders - insurers, providers, policymakers, and patients - to create a more sustainable and equitable healthcare future.
Read the Full Hartford Courant Article at:
https://www.yahoo.com/news/articles/ct-hospital-health-insurer-ink-090100053.html
on: Wed, Feb 25th
by: The Hill

on: Tue, Feb 24th
by: The Conversation

on: Mon, Feb 23rd
by: WCBD Charleston

on: Sat, Feb 21st
by: The Cool Down
on: Sat, Feb 21st
by: inforum
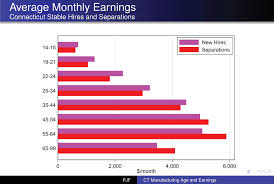
Connecticut Manufacturing Faces Critical Skilled Labor Shortage
on: Sat, Feb 21st
by: KMSP
UnitedHealthcare, Fairview Reach Deal, Averting Healthcare Disruption

on: Sun, Feb 15th
by: The Raw Story
Republican Healthcare Plan Faces Scrutiny Over Pre-Existing Condition Protections

on: Sun, Feb 15th
by: BBC

on: Fri, Feb 13th
by: BBC

on: Fri, Feb 13th
by: The Center Square

on: Thu, Feb 12th
by: NBC Connecticut
Hartford Nonprofit Faces Funding Shortfall Amid Rising Winter Need

on: Thu, Jan 22nd
by: Penn Live
UPMC-Highmark Contract Dispute Disrupts Healthcare in Pennsylvania