[ Sat, Mar 07th ]: ABC7

[ Sat, Mar 07th ]: WRDW

[ Sat, Mar 07th ]: NBC Connecticut

[ Sat, Mar 07th ]: NBC New York

[ Sat, Mar 07th ]: Erie Times-News
Pennsylvania Launches Program to Hire Displaced Federal Workers

[ Sat, Mar 07th ]: The Baltimore Sun

[ Sat, Mar 07th ]: Orange County Register

[ Sat, Mar 07th ]: KTLA
Clearwater Beach Bacteria Advisory Sparks Wider Coastal Concerns

[ Sat, Mar 07th ]: World Socialist Web Site

[ Sat, Mar 07th ]: Deadline
Film's Hotline Number Causes Real-World Crisis for Addiction Support Line

[ Sat, Mar 07th ]: Patch

[ Sat, Mar 07th ]: NBC News
RFK Jr. Fuels Debate on Alternative Therapies in Medical Schools

[ Sat, Mar 07th ]: Jerry

[ Sat, Mar 07th ]: ABC Kcrg 9

[ Sat, Mar 07th ]: Hartford Courant

[ Sat, Mar 07th ]: LA Times

[ Fri, Mar 06th ]: NBC Chicago

[ Fri, Mar 06th ]: Seattle Times

[ Fri, Mar 06th ]: Mediaite

[ Fri, Mar 06th ]: BBC

[ Fri, Mar 06th ]: Orlando Sentinel

[ Fri, Mar 06th ]: Newsweek

[ Fri, Mar 06th ]: Iowa Capital Dispatch

[ Fri, Mar 06th ]: The Boston Globe
CVS and Google Partner to Revolutionize Pharmacy Services with AI

[ Fri, Mar 06th ]: Post and Courier

[ Fri, Mar 06th ]: Popular Mechanics

[ Fri, Mar 06th ]: Medical News Today

[ Fri, Mar 06th ]: Sports Illustrated
Shae Cornette's Style Steals the Show on ESPN's *First Take*

[ Fri, Mar 06th ]: moneycontrol.com

[ Fri, Mar 06th ]: London Evening Standard
UK Government Faces Fire for Hosting Anti-LGBTQ+ Brazilian MPs

[ Fri, Mar 06th ]: MassLive

[ Fri, Mar 06th ]: Morning Call PA

[ Fri, Mar 06th ]: TwinCities.com

[ Fri, Mar 06th ]: Orange County Register
California's Medicaid Work Requirements Face Legal Challenge

[ Fri, Mar 06th ]: Washington Examiner
Surgeon General Nominee Faces Scrutiny Over Holistic Health Views

[ Fri, Mar 06th ]: Seeking Alpha

[ Fri, Mar 06th ]: NBC News

[ Fri, Mar 06th ]: WTOP News

[ Fri, Mar 06th ]: Chicago Sun-Times

[ Fri, Mar 06th ]: NBC 7 San Diego

[ Fri, Mar 06th ]: Total Pro Sports
Maxx Crosby Publicly Expresses Desire to Join Dallas Cowboys

[ Fri, Mar 06th ]: The New Indian Express

[ Fri, Mar 06th ]: CBS News

[ Fri, Mar 06th ]: Us Weekly

[ Fri, Mar 06th ]: Madison.com

[ Fri, Mar 06th ]: Boston Herald

[ Fri, Mar 06th ]: Fortune

[ Fri, Mar 06th ]: Fox 11 News

University of Chicago Study Favors Waist-to-Height Ratio Over BMI for Diabetes Risk
 Fox 11 News
Fox 11 NewsLocale: UNITED STATES




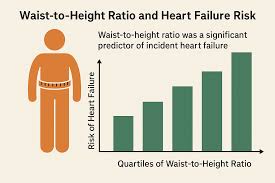
CHICAGO, IL - March 6th, 2026 - A groundbreaking study from the University of Chicago is poised to reshape how healthcare professionals assess and predict the risk of Type 2 diabetes. Published recently in Diabetes Care, the research highlights the limitations of the long-standing Body Mass Index (BMI) and champions the waist-to-height ratio (WHtR) as a more accurate and informative metric for identifying individuals at risk.
The BMI, a calculation based on weight and height, has been a cornerstone of public health screening for decades. However, critics have consistently argued that it fails to distinguish between muscle mass and fat, offering a potentially misleading assessment of an individual's health. The new University of Chicago study appears to bolster those criticisms, demonstrating that a higher waist-to-height ratio is a significantly stronger predictor of Type 2 diabetes development, even in individuals with a 'normal' BMI.
Dr. Christi Deaton, lead researcher on the study, explained the fundamental flaw with BMI: "We've known for some time that BMI isn't a perfect measure. It simply doesn't tell us where the fat is located on the body. This is crucial, because abdominal fat, often referred to as visceral fat, is far more metabolically active and strongly linked to insulin resistance - a key precursor to Type 2 diabetes."
The WHtR, calculated by dividing waist circumference by height, provides a simple yet powerful indicator of abdominal fat accumulation. Dr. Deaton's team meticulously analyzed data from over 2,000 adults, revealing a clear correlation between elevated WHtR and the incidence of Type 2 diabetes. The findings demonstrated that individuals with higher ratios were demonstrably more likely to develop the disease, regardless of their BMI classification. This suggests that a person could appear to be within a healthy weight range according to BMI, yet still harbor a significantly increased risk of diabetes if they carry excessive abdominal fat.
The implications of this research extend beyond individual health assessments. Experts believe that integrating the WHtR into routine public health screening programs could dramatically improve early detection rates and enable more targeted preventative interventions. "This isn't about replacing BMI overnight," clarifies Dr. Anya Sharma, an independent endocrinologist not involved in the University of Chicago study, "but it's a compelling argument for adding WHtR as a complementary metric. It provides a more nuanced picture of metabolic health and allows us to identify individuals who might be slipping under the radar with BMI alone."
The ease of calculation is another key advantage of WHtR. Unlike more complex measurements like DEXA scans or bioelectrical impedance analysis, WHtR requires only a simple tape measure and a height reading. This makes it easily implementable in a variety of settings, from primary care physician offices to community health fairs. The cost-effectiveness of the measurement is particularly appealing for resource-constrained healthcare systems.
The growing body of research supporting the WHtR is prompting a wider conversation about the limitations of relying solely on BMI. Several studies across different populations have consistently demonstrated its superior predictive power for cardiovascular disease, metabolic syndrome, and overall mortality. A 2024 meta-analysis published in The Lancet Diabetes & Endocrinology found that WHtR was a stronger predictor of diabetes risk than BMI in all ethnic groups studied.
However, some challenges remain. Standardization of measurement protocols is crucial to ensure accuracy and comparability of data. The position of the body during waist circumference measurement can influence the results, necessitating clear guidelines for healthcare professionals. Furthermore, research is ongoing to determine optimal WHtR thresholds for different populations and age groups.
Despite these challenges, the momentum behind the WHtR is undeniable. Dr. Deaton emphasizes, "It's about more than just the number on the scale. It's about the health implications of that weight and understanding where that weight is distributed. A healthy weight isn't just about aesthetics; it's about metabolic function and reducing the risk of chronic diseases like Type 2 diabetes." The University of Chicago team is now focusing on larger, long-term studies to further validate their findings and explore the potential for personalized interventions based on WHtR measurements. The future of diabetes risk assessment may well be shaped by a simple ratio that shifts the focus from overall weight to abdominal fat - a critical factor in metabolic health.
Read the Full Fox 11 News Article at:
https://fox11online.com/news/nation-world/uchicago-researcher-says-waist-to-height-ratio-beats-bmi-to-spot-diabetes-risk-university-of-chicago-cdc-
[ Thu, Mar 05th ]: WHIO
West Nile Virus Threat Surges: Officials Issue Urgent Warnings

[ Thu, Mar 05th ]: Patch
CDC Issues Health Alert: Lymphatic Filariasis Spread Concerns

[ Thu, Mar 05th ]: Georgia Recorder

[ Mon, Mar 02nd ]: news4sanantonio

[ Sat, Feb 28th ]: The Nation

[ Fri, Feb 13th ]: Reuters
Global Study Links Ultra-Processed Foods to Increased Disease Risk

[ Wed, Feb 04th ]: The Independent US

[ Mon, Jan 26th ]: Prevention

[ Sat, Jan 24th ]: MassLive

[ Wed, Jan 21st ]: TheHealthSite
India Faces Rising NCD Crisis: 60% of Deaths Now NCD-Related

[ Thu, Dec 04th 2025 ]: TheHealthSite
Diabetes Drives Rising Sudden Cardiac Death Risk in Young Adults
